The 3rd part of this series of naked tales of a studying physio picks up from where we left part 2. Here I talk about my observations and formulate my case for management. You can read parts 1 and 2 here and here.
Observations
Interestingly, as the patient walked into the examination room it was observed and noted that the patient had a mild ataxic gait. Further investigation of his medical history revealed no motor or cerebellar insult this was supported by a brain MRI in February 2015 which ruled out any indication of brain infarct.
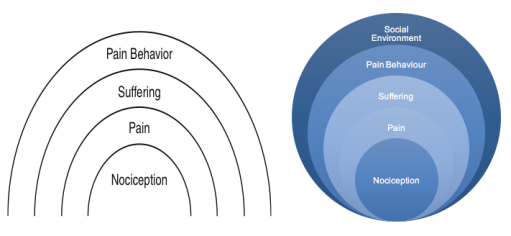
The presentation of the patient’s mild ataxia was discussed with the assessing psychologist and medical doctor. It was agreed that the continuation of a pain management program was appropriate considering the ataxic gait had been apparent since his injury and that major brain infarction had been ruled out. Furthermore, it was agreed that the ataxic gait may have been a result of excessive alcohol consumption or a pain behaviour as a result of operant conditioning. According to Fordyce’s (1979) behavioural model of pain, pain behaviours are influenced by three important factors: nociception, pain and suffering. Loeser (1982) further expanded Fordyce’s model to include social environment (Figure 4).
The screening exam included a neuromuscular examination of the lower extremities consisting of dermatomal sensation, myotomal strength, deep tendon reflexes and upper motor neurone testing, including Babinski and clonus. There were no abnormal findings with neurological testing. Further test of cerebellar function included heel shin test, rapid tapping of foot and finger nose test. Some slowness in movement was noted but no lack of co-ordination (Butler, 2000).
Spinal range of movement (cervical, thoracic and lumbar) was assessed with quick range of movement tests to peripheral joints including hips and shoulders to minimize exacerbation of pain.
Isolated strength testing had been conducted during neurological testing and as such task specific testing was conducted. A simple assessment of everyday tasks was performed. This included assessment of gait, sit to stand test, lifting test and lift and carry test. Testing was aimed at identifying pain behaviours and beliefs during activity and also obtain an objective baseline of physical exertion using the rate of perceived exertion scale (Borg, 1982).
Questionnaires
The patient was asked to complete the following screening questionnaires:
- Disability Anxiety Stress Scale
- Pain Catastrophising Scale
- Pain Disability Index
Each questionnaire was clinically justified from the subjective history and nature of the patient’s presentation, particularly drawn from his beliefs, anxiety and fear of movement.
Case Formulation
The case formulation is based upon information gathered from the case history. It aims to identify aspects of the patient’s experiences living with pain and appropriately apply a clinically reasoned hypothesis for management intervention. The case formulation is based upon Vertue & Haig’s (2008) Abductive Theory of Method (ATOM). Abductive reasoning is the inference of problem patterns that are observed in a person’s functioning to which a plausible explanation can be given (Vertue & Haig, 2008).
The case formulation is separated into the following:
Relatively Stable Phenomena
- Pain behaviours – breath holding, ataxic gait, tensing on movement, jaw contortion
- Pain related anxiety and avoidance
- Work disability
Biophysical
- Vertebral fractures at C1, C2 T4-T7
- Rib fractures including bilateral Rib 1
- Disc collapse and calcification T10/11
- Traumatic Brain Injury
- Central Sensitisation
Psychological
- Unhelpful beliefs about pain and activity
- Catastrophising
- Anxiety/stress about spine pathology
- Negative reinforcement from avoiding movements expected to be painful
- Issues with WC not providing funding for surgery
- Memory issues and frustration
Social
- Unhelpful explanations from treatment providers
- Isolating himself due to unemployment and living with father
- On long term compensation
- Cognitive overload in busy environments
Proximal causal factors
- Fall off bike causing disc collapse and calcification
Maintaining factors
Specialist perpetuating anxiety with fear inducing language
Case management not providing funding for required surgery
Anxiety and pain behavior reinforcing disability
Negative beliefs reinforcing fears and disability
Healthcare providers not providing adequate explanation to reduce fear and anxiety
Consideration of the relationships these factors can be demonstrated in the following diagram (Figure 5).
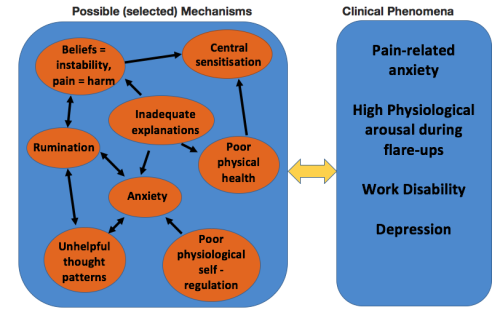
Vertue & Haig (2008) state, ‘case formulation is the culmination of the clinical reasoning process and is a comprehensive and, hopefully, integrated conceptualization of a case encompassing phenomenology, etiology, maintaining factors, prognosis, and treatment recommendations.’
In essence it provides a comprehensive hypotheses based upon a biopsychosocial framework to deliver appropriate management to a multidimensional problem such as persistent back pain. Intervention may include rehabilitation principles from physiotherapy to address the negative beliefs and behaviour about movement and poor physical health, psychology to apply cognitive behavioural approaches to challenge unhelpful thought patterns and occupational therapy to support the patient in return to work and social isolation.
A multi-disciplinary team (MDT) would collaboratively work with the patient to address many of the issues limiting his life through problem solving and goal setting. Furthermore, a significant factor that I believe has contributed to the patient’s low mood is the message from the orthopaedic specialist. Contact with the orthopaedic specialist to further discuss the evidence (or lack of) around benign spinal pathology and pain and the evidence for and against having spinal surgery in relation to the patients pathology would perhaps provide the patient with some reassurance about his injury.
Conclusion
The case report describes a complex case study of a patient living with a 5-year history of persistent back pain. The application of a case formulation process adopting a biopsychosocial framework aims to provide the clinician or MDT with the appropriate means to deliver a more comprehensive and effective management plan.
Albeit brief regarding intervention this case study is to demonstrate critical thinking in order to appropriately apply clinical reasoning for an intervention plan. The final part is still to come, which is my personal reflection on what I could have expanded on and discussed further. A 3000 word limit I have found can be somewhat restrictive.
I hope that this case study has provided an insight into the complexity of formulating an appropriate management plan using a BPS framework. I hope it brings some guidance to clinicians looking to venture into understanding the BPS model and the assessment criteria required for case formulation.
Thanks for having a read and watch out for part 4 next week.
TNP
References
Armon, C., Argoff, C. E., Samuels, J., & Backonja, M.-M. (2007). Assessment: use of epidural steroid injections to treat radicular lumbosacral pain. Neurology, 68, 723–729. http://doi.org/10.1212/01.wnl.0000256734.34238.e7
Barker, K. L., Reid, M., & Minns Lowe, C. J. (2009). Divided by a lack of common language? A qualitative study exploring the use of language by health professionals treating back pain. BMC Musculoskeletal Disorders, 10, 123. http://doi.org/10.1186/1471-2474-10-123
Barker, K. L., Reid, M., & Minns Lowe, C. J. (2014). What does the language we use about arthritis mean to people who have osteoarthritis? A qualitative study. Disability and Rehabilitation, 36(5), 367–372. http://doi.org/10.3109/09638288.2013.793409
Borg, G. A. (1982). Psychophysical bases of perceived exertion. Medicine and Science in Sports and Exercise, 14(5), 377–381. http://doi.org/10.1249/00005768-198205000-00012
Chou Roger , MD; Qaseem Amir , MD, PhD, MHA; Snow Vincenza , MD; Casey Donald , MD, MPH, MBA; Cross Jr J. Thomas ., MD, MPH; Shekelle Paul , MD, PhD; and Owens Douglas K. , MD, M. (2007). Clinical Guidelines Diagnosis and Treatment of Low Back Pain : A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society, (July 2007).
Clark, B. C., Goss, D. A., Walkowski, S., Hoffman, R. L., Ross, A., & Thomas, J. S. (2011). Neurophysiologic effects of spinal manipulation in patients with chronic low back pain. BMC Musculoskeletal Disorders, 12, 170. http://doi.org/10.1186/1471-2474-12-170
Darlow, B., Dowell, A., Baxter, G. D., Perry, M., Mathieson, F., Perry, M., & Dean, S. (2013). The Enduring Impact of What Clinicians Say to People With Low Back Pain. Annals of Family Medicine, 11(6), 527–534. http://doi.org/10.1370/afm.1518.INTRODUCTION
Deyo, R. a, Mirza, S. K., Turner, J. a, & Martin, B. I. (2009). Overtreating chronic back pain: time to back off? Journal of the American Board of Family Medicine : JABFM, 22(1), 62–68. http://doi.org/10.3122/jabfm.2009.01.080102
Eccleston, C., & Crombez, G. (2007). Worry and chronic pain : A misdirected problem solving model. Pain, 132(3), 233–236. http://doi.org/10.1016/j.pain.2007.09.014
Ferreira, M. L., Machado, G., Latimer, J., Maher, C., Ferreira, P. H., & Smeets, R. J. (2010). Factors defining care-seeking in low back pain - A meta-analysis of population based surveys. European Journal of Pain, 14(7), 747.e1–747.e7. http://doi.org/10.1016/j.ejpain.2009.11.005
Greville-Harris, M., & Dieppe, P. (2015). Bad is more powerful than good: The nocebo response in medical consultations. American Journal of Medicine, 128(2), 126–129. http://doi.org/10.1016/j.amjmed.2014.08.031
Hoffmann, T., Del Mar, C., Strong, J., & Mai, J. (2013). Patients’ expectations of acute low back pain management: implications for evidence uptake. BMC Family Practice, 14(1), 7. Retrieved from http://www.biomedcentral.com/1471-2296/14/7
Hoy, D., Bain, C., Williams, G., March, L., Brooks, P., Blyth, F., … Buchbinder, R. (2012). A systematic review of the global prevalence of low back pain. Arthritis and Rheumatism, 64(6), 2028–2037. http://doi.org/10.1002/art.34347
Hoy, D., March, L., Brooks, P., Blyth, F., Woolf, A., Bain, C., … Buchbinder, R. (2014). The global burden of low back pain: estimates from the Global Burden of Disease 2010 study. Annals of the Rheumatic Diseases, 73(6), 968–974. http://doi.org/10.1136/annrheumdis-2013-204428
Kamper, S. J., Apeldoorn, A. T., Chiarotto, A., Smeets, R. J. E. M., Ostelo, R. W. J. G., Guzman, J., & van Tulder, M. W. (2015). Multidisciplinary biopsychosocial rehabilitation for chronic low back pain: Cochrane systematic review and meta-analysis. BMJ (Clinical Research Ed.), 350(February), h444. http://doi.org/10.1136/bmj.h444
Kumar, S., Beaton, K., & Hughes, T. (2013). The effectiveness of massage therapy for the treatment of nonspecific low back pain: a systematic review of systematic reviews. International Journal of General Medicine, 6, 733–41. http://doi.org/10.2147/IJGM.S50243
Liddle, S. D., Baxter, G. D., & Gracey, J. H. (2007). Chronic low back pain: patients’ experiences, opinions and expectations for clinical management. Disability and Rehabilitation, 29(776008562), 1899–1909. http://doi.org/10.1080/09638280701189895
Linton, S. J. (2000). A review of psychological risk factors in back and neck pain. Spine (Phila Pa 1976), 25(9), 1148–1156. http://doi.org/10.1097/00007632-200005010-00017
McBeth, J., & Jones, K. (2007). Epidemiology of chronic musculoskeletal pain. Best Practice & Research. Clinical Rheumatology, 21(3), 403–25. http://doi.org/10.1016/j.berh.2007.03.003
Nijs, J., Roussel, N., van Wilgen, P. C., Koke, A., & Smeets, R. (2013). Thinking beyond muscles and joints: Therapists’ and patients’ attitudes and beliefs regarding chronic musculoskeletal pain are key to applying effective treatment. Manual Therapy, 18(2), 96–102. http://doi.org/10.1016/j.math.2012.11.001
O’Keeffe, M., Purtill, H., O’Sullivan, P., Dankaerts, W., Conneely, M., Hurley, J., … O’Sullivan, K. (2015). Comparative effectiveness of active interventions for non-specific chronic spinal pain: Physical, behavioural or combined? A systematic review and meta-analysis. Physiotherapy (United Kingdom), 101, eS1131–eS1132. http://doi.org/10.1016/j.jpain.2016.01.473
Ramond, A., Bouton, C., Richard, I., Roquelaure, Y., Baufreton, C., Legrand, E., & Huez, J. F. (2011). Psychosocial risk factors for chronic low back pain in primary care-a systematic review. Family Practice. http://doi.org/10.1093/fampra/cmq072
Skelton, J. R., Wearn, A. M., & Hobbs, F. D. R. (2002). A concordance-based study of metaphoric expressions used by general practitioners and patients in consultation. British Journal of General Practice, 52(475), 114–118.
Sullivan, M. J. L., Bishop, S. R., & Pivik, J. (1995). The Pain Catastrophizing Scale: Development and validation, 7(4), 524–532. Retrieved from http://www.scopus.com/inward/record.url?eid=2-s2.0-0029584617&partnerID=40&md5=7f8615d1b52cbabde152c2e9b9683fff
Tait, C.R. Pollard, C.A. Margolis, R.B. Duckro, P.N. Krause, S. J. (1987). The Pain Disability Index: Psychometric and Validity Data. Archives of Physical Medicine and Rehabilitation.
Thomas, E. N., Pers, Y. M., Mercier, G., Cambiere, J. P., Frasson, N., Ster, F., … Blotman, F. (2010). The importance of fear, beliefs, catastrophizing and kinesiophobia in chronic low back pain rehabilitation. Annals of Physical and Rehabilitation Medicine, 53(1), 3–14. http://doi.org/10.1016/j.rehab.2009.11.002
Vertue, F. M., & Haig, B. D. (2008). An Abductive Perspective on Clinical Reasoning and Case Formulation. Journal of Clinical Psychology, 64(9), 1046–1068. http://doi.org/10.1002/jclp
Vlaeyen, J. W. S., & Linton, S. J. (2000). Fear-avoidance and its consequences in chronic musculoskeletal pain: A state of the art. Pain, 85(3), 317–332. http://doi.org/10.1016/S0304-3959(99)00242-0
Vos, T., Flaxman, A. D., Naghavi, M., Lozano, R., Michaud, C., Ezzati, M., … Moradi-Lakeh, M. (2012). Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: A systematic analysis for the Global Burden of Disease Study 2010. The Lancet, 380(9859), 2163–2196. http://doi.org/10.1016/S0140-6736(12)61729-2
Walsh, D. A., & Radcliffe, J. C. (2002). Pain beliefs and perceived physical disability of patients with chronic low back pain. Pain, 97(1-2), 23–31. http://doi.org/10.1016/S0304-3959(01)00426-2
Xu, N., Wei, F., Liu, X., Jiang, L., & Liu, Z. (2016). Calcific discitis with giant thoracic disc herniations in adults. European Spine Journal, 1–5. http://doi.org/10.1007/s00586-016-4402-y
Yelland, M. (2011). What do patients really want to know? International Musculoskeletal Medicine, 33(1), 1–2.


Hi Paul
Thank you for the very informative blog about this patient who is any (mortal) physio’s idea of a challenge. It seems clear that the patient does have significant persistent pain problem with sub-optimal coping strategies and it appears that the level of rehabilitative input had been nothing short of comprehensive. If I may be able to speculate a little bit here, has it been considered or confirmed that this patient’s problem is also likely to be a developing central canal stenosis of the thoracic spine secondary to post-traumatic degenerative changes which would account for his ataxia (even in the apparent abscence of long tract sign) ? I am reading between the lines based on the orthopaedic surgeon’s somewhat pessimistic outlooks to the patient’s prognosis and the offer for surgery to prevent further deterioration which in most cases is the most commonly proposed outcome for decompression/fusion surgery. The patient’s interpretation, as you have outlined, appears to be somewhat skewed although not grossly misled. As a clincian with a foot in the biomedical and biopsychosocial camps, it seems a tricky situation to me to provide the patient with realistic expectation towards his/her outcome especially when there is a potential likelihood of true physiological disability (stenosis with possible myelopathy) while taking into account the patient’s perception of the information which he/she receives. I woud appricate your input regarding this particular scenario. Again, my apology if this seems highly speculative.
Cheers
Michael.
LikeLike
Hi Michael,
Thanks for the message and certainly I would agree with your suspicions, it is something I raised with the orthopaedic surgeon and medical doctors who examined the patient and felt there were no grounds for this according to their findings and the accompanying CT and MRI scan. I questioned whether the patients ataxia was due to the sustained mild head trauma. This had been investigated and no probable cause was found. I assessed fine motor function, heel/shin, finger nose, alternating hand and neurological testing appeared clear. I understand that he is awaiting an assessment from the public health system. Thank you for your input and feedback, I will raise this once again with his specialist.
LikeLike
Thank you Paul. I am being a casual observer making bold comments. Hope all goes well for this gentleman.
LikeLike
Thanks Michael,
I don’t think your comments are bold, more completely appropriate. I admit I have on occasion swung the pendulum to far to be be brain bound and not still consider the biological and structural changes. Despite evidence highlighting myelopathy prevalence in asymptomatic patients I still think we need to consider what is presented in front of us. Thanks again for you comment, much appreciated.
LikeLike
May I add that a number of patients with symptomatic myelopathy can be asymptomatic piror, hence the common presentation of sudden deterioration of sensorimotor function. The usual course of symptomatic myelopathy is more progressive and gradual. I seem to struggle a bit to track down prevalence of asymptomatic myelopathy. Asymptomatic spinal stenosis with cord compression without myelopathy is perhaps more prevalent. It’s a moot point as in clinical practice, myelopathy is often symptomatic prior to imaging. Hoever, I have digressed.
LikeLike
Hi everyone, it’s my first go to see at this website, and
article is in fact fruitful in support of me, keep up posting these content. http://Marinsbertoldi.Com.br/
LikeLike
This article wilol hdlp the internet viewers for building
upp new web site oor even a weblog rom start to end.
LikeLiked by 1 person