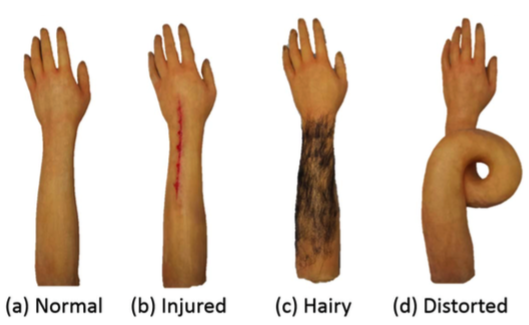
Complex Regional Pain Syndrome (CRPS) is an incredibly debilitating condition. It effects the peripheral limbs specifically the hands and feet. CRPS usually occurs following trauma to the limb, commonly a fracture but also sprains, strains and crush injuries (Bruehl, 2015). It has also been recorded to occur following minor trauma such as a bee sting (Birklein & Rowbotham, 2005). It’s characterized by a cluster of symptoms that include the cardinal signs of inflammation, trophic changes such as increased hair and nail growth, changes in sensitivity which include hyperalgesia and allodynia or sensitivity to normally non-painful stimuli such as movement, touch and temperature.
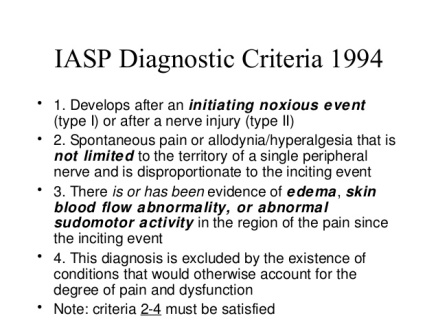
There are a specific set of criteria to help to ascertain if someone has CRPS, called the Budapest criteria, it was developed by the International Association for the Study of Pain (IASP) and is an update to the old criteria developed by Merskey & Bogduk (Eds), (1994).
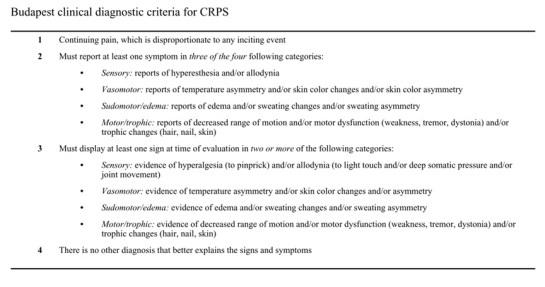

Now I wouldn’t call myself an expert in CRPS, however I do believe that if there are a specific set of criteria to assist with confirming CRPS then any assessment should be made with strict respect for the criteria. Update (2018) - ‘A more recent survey of practitioners found that a large proportion of clinicians are not using the internationally recognised criteria (Miller et al., 2017). I am seeing more and more people being labelled with CRPS when I would say they don’t meet the Budapest criteria. To my knowledge there is no evidence to support a diagnosis of “mild CRPS” or shows “vague symptoms of CRPS”. In addition, I have seen some patients diagnosed with CRPS of other body parts including shoulders, elbows, and even the back and yet there is limited evidence if any to confirm CRPS could exist in these body parts.
The Budapest criteria isn’t flawless yet it was developed to do away with this issue. The original IASP criteria lacked specificity and validity in the diagnostic process of defining CRPS and as such many people were misdiagnosed with CRPS. Furthermore, people were being diagnosed as a result of expressing one or two signs and/or symptoms of CRPS and yet CRPS is an interaction of mechanisms ranging from several components to determine its aetiology (Harden et al., 2010). Interestingly, the incidence of diagnosed CRPS reduced significantly following the development and release of the Budapest criteria (Birklein & Schlereth, 2015).
My concern is when an individual is given a diagnosis of CRPS because 1) they continue to report pain in their affected limb after a prolonged period of time 2) Are still searching for a diagnosis and 3) do not specifically show other signs of CRPS based on the IASP criteria.
It is fair to say that there is a small amount of research that has suggested an additional category of CRPS. The not otherwise specified or CRPS-NOS category. It has been proposed that this category would be intended for people who “partially” fit the criteria. There are implications as a result with the main being that CRPS would become a label and not a diagnosis.
Personally, I don’t think lazy labelling should be substituted for diagnostic rigor. The diagnosis of CRPS is purely clinical and as it currently stands should meet the standards set by the Budapest criteria. Clinicians can deliver specific sensory testing including two-point discrimination, light and crude touch as this helps to determine cortical re-organisation (Flor, Nikolajsen, & Staehelin Jensen, 2006; Maihöfner, Handwerker, Neundörfer, & Birklein, 2003; G. L. Moseley & Wiech, 2009) which is commonly associated with CRPS. We can use hand laterality recognition (L. G. Moseley, Butler, Beames, & Giles, 2012) and probably not used as much (but should be used more) is quantitative sensory testing (QST) and skin conductance to assist with supporting a diagnosis of CRPS (Maier et al., 2010; Rommel, Malin, Zenz, Jänig, & Janig, 2001). QST is something that I will be investigating in a future blog.
Further assessment procedures can come from imaging such as MRI or x-ray but both have poor sensitivity and specificity and 3 phase bone scan scintigraphy only showed moderate specificity (Birklein & Schlereth, 2015) and is not part of the IASP criteria . Thermography is another method to identify temperature changes in the limb, nerve conductions and blood serum tests are also helpful for ruling out other potential conditions that may present with similar characteristics. This includes rheumatological conditions such as RA or neuropathies because of trauma.
In summary, CRPS is a complex and debilitating condition. It is of the upmost importance that when it comes to diagnosing CRPS that a label is not slapped on the patient to provide them with a diagnosis. This could lead to more serious implications for the patient. A CRPS diagnosis should be made by a specialized multi-disciplinary team taking into account the mechanisms that make up the complex condition. This way a collaborative formulated approach can be delivered and implemented when it comes to rehabilitation.
Thanks for having a read
TNP
References
Birklein, F., & Rowbotham, M. C. (2005). Does pain change the brain? Neurology, 65(5), 666–667. https://doi.org/10.1212/01.wnl.0000179148.80687.f3
Birklein, F., & Schlereth, T. (2015). Complex regional pain syndrome-significant progress in understanding. Pain, 156 Suppl, S94-103. https://doi.org/10.1097/01.j.pain.0000460344.54470.20
Bruehl, S. (2015). Complex regional pain syndrome. British Medical Journal, 350. https://doi.org/10.1136/bmj.h2730
Flor, H., Nikolajsen, L., & Staehelin Jensen, T. (2006). Phantom limb pain: a case of maladaptive CNS plasticity? Nature Reviews Neuroscience, 7(11), 873–881. https://doi.org/10.1038/nrn1991
Harden, R. N., Bruehl, S., Perez, R. S. G. M., Birklein, F., Marinus, J., Maihofner, C., … Vatine, J. J. (2010). Validation of proposed diagnostic criteria (the “budapest Criteria”) for Complex Regional Pain Syndrome. Pain, 150(2), 268–274. https://doi.org/10.1016/j.pain.2010.04.030
Maier, C., Baron, R., Tölle, T. R., Binder, A., Birbaumer, N., Birklein, F., … Treede, R. D. (2010). Quantitative sensory testing in the German Research Network on Neuropathic Pain (DFNS): Somatosensory abnormalities in 1236 patients with different neuropathic pain syndromes. Pain, 150(3), 439–450. https://doi.org/10.1016/j.pain.2010.05.002
Maihöfner, C., Handwerker, H. O., Neundörfer, B., & Birklein, F. (2003). Patterns of cortical reorganization in complex regional pain syndrome. Neurology, 61(12), 1707–1715. https://doi.org/10.1212/01.WNL.0000098939.02752.8E
Merskey, H., & Bogduk (Eds), N. (1994). Classification of Chronic Pain. Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms. IASP Press, i–xvi. https://doi.org/10.1002/ana.20394
Miller, C., Williams, M., Heine, P., Williamson, E., & O’Connell, N. (2017). Current Practice in the Rehabilitation of Complex Regional Pain Syndrome: A Survey of Practitioners. Disability and Rehabilitation. DOI: 10.1080/09638288.2017.1407968
Moseley, G. L., & Wiech, K. (2009). The effect of tactile discrimination training is enhanced when patients watch the reflected image of their unaffected limb during training. Pain, 144(3), 314–319. https://doi.org/10.1016/j.pain.2009.04.030
Moseley, L. G., Butler, D. S., Beames, T. B., & Giles, T. J. (2012). The Graded Imagery Handbook. Retrieved from http://books.google.com/books?hl=en&lr=&id=hh5lMD4DMakC&oi=fnd&pg=PP7&dq=graded+motor+imagery&ots=SKcSXWI_OK&sig=Hs8w32culWcE-9iuDaw2b-Sc_EY%5Cnpapers2://publication/uuid/FB7E5C78-5A23-40C1-B8D0-80848B8FF2C4
Rommel, O., Malin, J.-P. P., Zenz, M., Jänig, W., & Janig, W. (2001). Quantitative sensory testing, neurophysiological and psychological examination in patients with complex regional pain syndrome and hemisensory deficits. Pain, 93(3), 279–293. https://doi.org/http://dx.doi.org/10.1016/S0304-3959(01)00332-3

Totally agree. I feel the proliferation of quasi-CRPS diagnoses (backs, visceral) may be a way of giving a label. However, I would contend the more appropriate label is simply chronic pain with central sensitization, as it is typically the allodynia, hyperalgesia and summation features that map onto the Budapest criteria.
LikeLiked by 1 person
Hi Tara
Thanks for your comment and agree with your point you make. I admit I have found people have difficulty accepting chronic pain with central sensitisation because it does not fit with the body as machine metaphor and the need to see what is wrong with them from a tissue perspective. Still much work to do!
LikeLike
I was diagnosed with CRPS 1 20 years ago in my right arm following a right rhomboid tear. It exited into Microsoft cloud and then reentered my body by accident in my left arm, mirroring the pain in my right arm, but to a lessor degree. My doctor ended up giving the right arm a nerve block, which magically (blessedly) fixed the left arm as well. I soon went on my way, assuming that when my doctor healed my arm he healed the RSD as well.
Now, 20 years later, I strained my right lower back. My right foot was on fire and felt crushed by the weight of the bedsheet. My calf was untouchable. Over the months the extreme pain went up my back and into my neck, giving me migraines. It then crossed over to the left side and began to exactly mirror the pain on the right. I felt my body was possessed. I had to constantly fight having a panic attack caused by the conflict of wanting to leave my terrifying body and knowing I could not do so. My doctor told me I may need surgery on my neck, and I made a beeline 1200 miles to the doctor of 20 years ago because I wanted an osteopathic opinion, and he was the only osteopathic I know. That’s when I found out CRPS doesn’t go away. That was 4 months ago, in August, 4 months after the injury. So he gave me a sphenopalatine block, a caudal epidural, trigger point injections, and some osteopathic moves and I left his office totally pain free and as limber as my kitten. After 9 plus days of bliss the pain started coming back from the feet up without missing any spots. It got to my chest and I returned to him in October. This time the pain was beat back. It was tolerable for a while, but has been slowly increasing in intensity. Unable to find help close to home (because the doctors don’t see the Budapest criteria so they want diagnosed it and treat it. Why don’t they see it? Because it’s partially treated.), last week, after not sleeping for 3 nights due to the pain, I went to a university ER 2 hours away and found help. I took my pile of MRI and test results and gave them their choice of diagnosis. I told them my story, they did great assessments and told me presentation was “classic CRPS”.
So for over 2 more months I’ve been in agony because the doctors don’t see the Budapest criteria fulfilled in a patient with a previous history of CRPS, in which the disease is partially treated after a remanifestation of the disease.
My point is this -what has happened to our value of common sense and intuition?
There’s a good reason this disease is called the “suicide disease”. Put together a systemic disease whose main manifestation is severe pain, with the random fight or flight responses which that disease causes, and top it off with caregiver neglect and abuse and you, may understand why much of rsda’s funding comes from families of CRPS patients who have murdered themselves.
In spite of what all that probably sounds like, I truly appreciate all you do and am glad I stumbled across your blog. CRPS is a systemic disease, not a ‘pain syndrome’. Each person is an enfleshed soul. The soul is expressed through the body, mind, spirit and relationships of the person. Because the SNS is so intimately involved in this disease, the most effective treatment for a person is the one that person believes in, given to that person by a caregiver they trust. Suppress faith and damage the ability to trust and you diminish outcomes.
God bless and Merry Christmas!
LikeLiked by 2 people
Hi Susan
I can only say that I can only imagine how hard it must be for you. I have worked with many people with CRPS and every single person is different. Medicine unfortunately groups us into buckets due in part to the limitation of treatment. You are absolutely right when it comes to believing in treatment. There is much research around expectations and beliefs.
Thank you for your kind words regarding my blogposts. I intend to bring many more on CRPS in the new year. I hope you have a Happy Christmas and a wonderful New Year.
Best wishes
Paul
LikeLiked by 1 person