The placebo effect is a fascinating area of medicine. In clinical trials the placebo- controlled trial is regarded as “the gold standard” to determine the efficacy of active treatments such as in a new drug. However, placebo doesn’t come without controversy particularly in areas of clinical practice such as the use of acupuncture, which is commonly used by Allied Health Professionals. Anyway rather than me launch into a romantic play works about placebo I thought I would let another physio have a crack at giving his thoughts on the topic. Take it away David Poulter.
Cogito ergo sum: I think therefore I am……susceptible to the non specific effects of placebo and nocebo.
“You can remove the active treatment effect from a placebo, but you can’t remove the placebo effect from an active treatment” – Poulter 2017
Placebo (Latin for I will please). In medicine a placebo is an inert substance, simply put “Nothing” it has no specific effects. Placebos are often used in pharmacy trials to compare a drugs presumed “active or specific” effect against a pill (sugar pill) with no active or specific effects, to help determine the real effect of the active drug.
In some studies, the use of a placebo (nothing) isn’t possible so instead a “sham” procedure is used, this is not to be confused with a placebo. A sham differs in that is included all the rituals and procedures involved in the real treatment, even to the point in sham surgery of cutting the skin and introducing arthroscopic probes. The sham though does not involve the active process of addressing the suspected pathology. Shams are often used in physical modality studies like acupuncture, taping, therapeutic ultrasound and surgery.
Shams actually hold the answer to why a placebo may have what appears to be an active or specific effect on the patients condition. This effect is is know as the “placebo effect”
So how can “nothing” have an effect? The answer is simple, it can’t.
“What?”, I here you say, “so what is the placebo effect?”
The placebo effect is the “non specific” effects in the patients reporting of symptoms or wellbeing. (Note reporting is the key word). Non specific effects are those that change things like pain, fear, feeling of well being, catastrophizing. What they are not, are changes in the physical underlying pathology i.e they don’t shrink cancerous tumors, or change pathological changes in joints.
So back to, how can nothing produce any effects on the patient? The answer lies in priming, context, ritual, the patient clinician interaction, patient expectations and beliefs. It has been suggested to stop the confusion of attributing non-specific effects to “nothing” (placebo) and re-labelling the effects as “contextual effects” (Kamper & Williams, 2013).
So, before we go further let’s just mention a little about priming and patient expectations. There have been two recent studies that suggest that “open placebo” is effective in treating irritable bowel syndrome (Kaptchuk et al., 2010) and chronic low back pain (Carvalho et al., 2016), both studies run by the same group using similar methods to administer the placebo. (More on the studies here and the problems with them.)
How is it possible for an open placebo (nothing), where patients are told they are receiving a sugar pill to have an effect, after I have just said that a placebo needs priming and context? Well, the study involved priming and hence the patients were actually being deceived and their expectations manipulated. This is not the same as saying here is an ineffective sugar pill which will have no effect.
Here is the information the patients in the study received:
“placebo pills, something like sugar pills, have been shown in rigorous clinical testing to produce significant mind-body self-healing processes.”
“either placebo (inert) pills, which were like sugar pills which had been shown to have self-healing properties” or no-treatment.”
As you can see, the patients were clearly primed and hence the treatment received was no longer an inert placebo, but a strongly influenced contextual effect that possibly could and actually did influence the patients expectations.
Priming, context and patient expectations may also be important for other reasons, the placebo effect is not the only non-specific effect linked to treatment and research (See here)
The most common non-specific effects which are often mistaken for the placebo effect are regression to the mean and natural resolution.
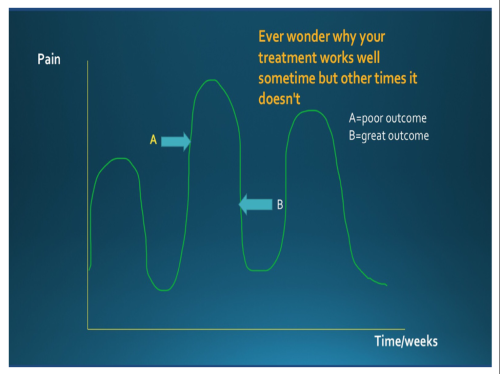
Simply put most conditions have times when they are worsening and times when they are getting better on their own. We need to be aware of this and not confuse these natural fluctuations in a condition and attribute them to our treatment.
Yesterday whilst pondering on writing this blog, (actually truth be told, after writing two other drafts of this blog) I posted this on twitter.
“Placebo=nothing, inert substance”
A placebo without priming or context = nothing, no effect.
Placebo effects are hence contextual effects produced by priming and context.
Proposal: let’s stop asking should we embrace placebo that is like asking should we embrace nothing.”

The reason I posted it was two-fold, one to see if I got the usual twitter kick back, and secondly because I believe it is time to get the message out that Physiotherapists do not need to embrace placebo. Remember placebo is technically nothing. What we may need to do is embrace the contextual factors which lead to the non-specific effects in our patients (Lucassen & Olesen, 2016)
The paper, Context as a drug: some consequences of placebo research for primary care by Lucassena & Olesen states the following in it’s conclusion.
‘The quality of the doctor–patient relation does matter. Words matter. Choices matter. Expectations matter. Atmosphere and behavior matters. One could also say: context matters. Placebo–nocebo research provides strong evidence for this link.
The therapeutic context induces processes that enhance or reduce the effects on symptoms of our interventions (drugs, surgery or cognitive behavioral therapy.)’
This implies the minute we interact with a patient, everything has an effect, be it positive or negative. (The placebo effects ugly cousin is the “nocebo effect” this is when, due to non-specific effects, the patient reports worsening of their pain or wellbeing)
I have proposed that TENS should be every clinician’s first contact treatment intervention. To initiate the positive contextual effects at the start of patient therapist interaction.

Remember everything matters, your therapeutic ritual, ability to listen, empathize, educate, interview, care, and the clinic environment are all contributing to the contextual effect of your treatment.
Thought:
Most of us pride ourselves on offering, what we consider, beneficial treatment to our patients. We share in the collective joy of watching someone who is in pain and lacking function, recover in our care. Although, we also experience those who don’t seem to get long term relief and struggle to regain function. We tend to move the non-responders on, often with negative messages like “we have done all that we can” or “you may need more than Physio can offer”. In our minds, we convince ourselves we care and that we help all who enter our clinic. But, what if we are wrong and that our behaviors, attitude, rituals, practice context, personality, ability to listen, empathize, and our style of patient education are having more effect (both positive and negative) on our patients than we realize? What if those who get better (and we revel in their success) just get better on their own, and those who don’t get better, don’t because of the way we interact with them? Is this something we should consider?
Are we part of the solution, or are we part of the problem?
Perhaps if we are going to take shared credit for a patient’s success, we may also need to take shared responsibility for their treatment failures too?
I have a favorite saying “offer patients solutions to their problems, not more problems” Are we treating all of our patients the same? Is our interaction with some patients a placebo effect whilst with others a nocebo effect? (both being contextual effects). Do we even consider this a possibility?
There are questions being asked from some in the Physiotherapy (Physical Therapy) profession about whether we should embrace and maximize the placebo effect in patient care? I think we should consider a bigger perspective, and ask “are we maximizing the positive contextual effect in patient care (which include placebo) whilst minimizing the negative contextual effects (nocebo)?” As a profession we must also be cognizant of the need to identify the specific treatment effect of our interventions, via evidence based research, otherwise we will be accused of being no better than placebo or contextual effects.
At this point you may be thinking why does it matter if we are no better than placebo or contextual effects? The answer is simple, placebo and contextual effects have limited to no effect on specific pathology. Remember they have an effect on the “subjective” elements of conditions such as pain, fear, anxiety, kinesiophobia and catastrophizing.
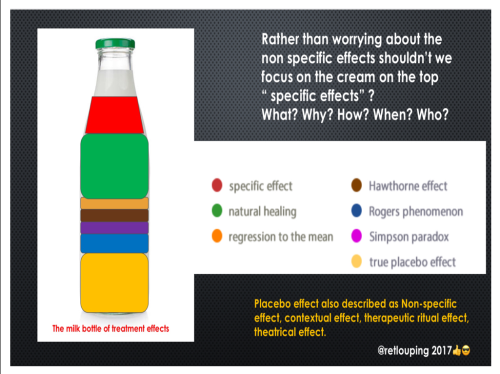
Proposal: Let’s maximise the positive contextual effect, eliminate the negative contextual effects and continue to provide treatment that has known specific effects.
This proposal has been drawn from an interesting and insightful read here.
I don’t want this blog to be too long or boring, I just want it to stimulate your interest and perhaps challenge you to read more and question the use of the term “placebo effect”.
So, in closing here are some things to consider.
- Is it time to abandon the term “placebo effect”?
- Can I maximise my positive contextual effects with my patients? (The artist formally known as placebo effect)
- Can I minimise the negative contextual effects with my patients? (The artist formally known as nocebo effect)
- Can we stop saying lets embrace placebo? (Not sure you can actually embrace nothing)
- Can I identify evidence based treatments that have specific effects on my patients?
Further watching and reading
Here are some interesting videos to watch on the placebo effect including surgery. (They may need to rename them “contextual effects” and sham procedures.)
Here is a link to the study mentioned in the videos: http://www.nejm.org/doi/pdf/10.1056/NEJMoa013259
So there you have it, accentuate the positive contextual effects in your daily interactions with your patients and eliminate the negative. Remember it’s important for the patient to understand and receive your message. Patient expectations are also part of the non specific effect (see here)
A great quote from the paper in the link:
“What we believe we will experience from a treatment our expectation has a substantial impact on what we actually experience. Expectation has been established as a key process behind the placebo (contextual effects) effect.”
Expectation has an important place in the response to “real” treatment as well.
“you can take the active treatment effect out of a placebo (nothing), but you can’t take the non specific effects (context and expectations) out of and active treatment. So why not maximise that effect?”
Here are some things to consider to maximise the contextual effects “The Seven Habits of Highly Effective Therapists”

Thanks for reading. Be kind to your patients and yourself.
Thanks again to David Poulter for sharing his insights and some of the evidence around placebo. It’s important that we all consider how we interact with our patients and how much of an influence that can have upon them positively or negatively. You can reach David on twitter @retlouping
TNP
References:
Carvalho, C., Caetano, J. M., Cunha, L., Rebouta, P., Kaptchuk, T. J., & Kirsch, I. (2016). Open-label placebo treatment in chronic low back pain: a randomized controlled trial. Pain, 157(12), 2766–2772. https://doi.org/10.1097/j.pain.0000000000000700
Kamper, S. J., & Williams, C. M. (2013). The placebo effect: powerful, powerless or redundant? British Journal of Sports Medicine, 47(1), 6–9. https://doi.org/10.1136/bjsports-2012-091472
Kaptchuk, T. J., Friedlander, E., Kelley, J. M., Sanchez, M. N., Kokkotou, E., Singer, J. P., … Lembo, A. J. (2010). Placebos without deception: A randomized controlledtrial in irritable bowel syndrome. PLoS ONE, 5(12). https://doi.org/10.1371/journal.pone.0015591
Lucassen, P., & Olesen, F. (2016). Context as a drug: some consequences of placebo research for primary care. Scandinavian Journal of Primary Healthcare, 34(4), 428–433. https://doi.org/10.1080/02813432.2016.1249065

Great post David, how about running an experiment for lets say low back pain where one group is given these contextual factors such as empathy you talked about but no further intervention and the other group given these contextual factors plus any intervention of our choice. Do you know of any studies like that, what were the results.
LikeLiked by 1 person
Some great points here and I agree with the general gist. Empathy can really go a long way I think - I have a wonderful GP who makes me laugh and makes me feel like a really valued person, and as if she cares about me. I always come away feeling tons better, even if she’s not actually been able to do much! On the contrary, I’ve had many an experience that went the opposite way, when I felt misunderstood, judged, not cared about etc.
I’m sorry to say that, overall, all of my experiences with physios were negative. Some were certainly nice, caring people but I usually came away in great pain (especially following ‘strength tests’, which seem very arbitrary and unnecessary in many cases!) and with a list of exercises which didn’t seem help at all. Looking back, I wasn’t even that clear what the point of the exercises was, compared to just going for a walk or doing some cleaning or cooking, which would have been far more enjoyable and useful. What actually happened was that I did their exercises then was in severe pain and dropped the cooking/cleaning/going out as a result.
None of them used the standard pacing technique, all went too fast, and in every case I discharged with the feeling that I had failed and I was defective and had wasted a lot of time and, in some cases, money. Unfortunately, while telling a patient things like ‘this won’t hurt’, ‘this will help you be in less pain’, or ‘you’ll be back cycling in no time’ may have some positive effect on expectations (as you describe), if the patient has an opposite experience such things will destroy the patient’s trust in the physio and potentially cause the patient to feel wrong/defective/a failure.
None that I saw before my diagnosis with Ehlers Danlos III suspected it either. And the ones after diagnosis didn’t really seem to understand the condition.
It’s great to be able to communicate with physios like you and hopefully this interaction will lead to better results for patients and physios alike.
You might be interested to check out my site as there are articles on physio and chronic pain on there. I’d love to get your thoughts.
LikeLiked by 1 person
Good article. I think two quotes sum it up quite well. “You can remove the active treatment effect from a placebo, but you can’t remove the placebo effect from an active treatment” – Poulter 2017 All treatments, indeed all interactions between a therapist/educator and a patient/client have placebo/nocebo effects or what David calls contextual effects. For the “placebo” I think part of this may be due to a shifting from sympathetic to parasympathetic dominance from the feeling of safety and being cared for (listened to, touched etc.).
The second is “What we believe we will experience from a treatment our EXPECTATION has a substantial impact on what we actually experience. Expectation has been established as a key process behind the placebo (contextual effects) effect.” I think expectation not only has a “placebo” effect but can trigger actual healing processes within the individual. Sometimes it is rather easy to understand as when a person with a sore back learns that the pain is not structural and starts moving more and the movement effects the healing. Just because some healing mechanisms are not as well understood doesn’t mean they don’t exist. We should never underestimate the power of expectation as a precursor to physiological events.
LikeLike