I’ve pondered for quite some time if we can efficiently tailor exercise programs for people living with pain.
Recent evidence (Hodges, 2019)and a consensus amongst peers, suggest that a hybrid approach to pain management programs is necessary. As proposed by Hodges, (2019) this would include stratification, identification of pain mechanism and subgrouping based on movement and/or psychology.
The multidimensional nature of chronic pain would certainly encourage those physiotherapists working in pain management to adopt a hybrid approach. The very nature of physiotherapy is to support a re-enablement to healthy or healthier living following injury or disease. One such avenue physiotherapists do this is through exercise.
Specifically to pain management programs, a common exercise approach is use of graded activity or graded reactivation (Figure 1). Based on a model of operant learning individuals work towards a quota of exercise and build physiological tolerance on a time contingent basis. The aim, to reinforce well behavior and recognizing that as quota’s increase individuals will adapt to the increasing demand (Fordyce, 2015). Essentially this represents the principle of specific adaptation of imposed demands or SAID principle.

Part of the graded activity approach is reinforcing the message hurt is not equal to harm, implying that pain does not mean tissue damage. Accepting the reality of this statement can be challenging for the person living with pain, particularly in the presence of a flare up. In addition, my experiences of patients living with pain is they often acknowledge that they are not concerned about doing more damage, it’s because they don’t want to experience pain, often because of the disruption it causes in their lives.
Considering a case formulaic approach (you can read about it here), I decided to investigate if, using exercise training principles, there was a more efficient way to develop exercise programs based upon the selected mechanisms and clinical phenomena that may lead to flare up following graded activity.
Case formulation can be delivered through various frameworks, but key features include:
- Identification and description of the presenting problems
- Factors that can lead to a sense of vulnerability or be causal to the problem
- Factors that are maintaining the problem, but may not have been part of the initial development of the problem
- Current coping strategies
As you will see later, I hope to provide an exercise program based on training principles utilizing a case formulaic approach.
Exercise Principles
The volume of evidence based material spanning principles of exercise training is vast. Of particular interest and covered in this blog includes individualization, rate of perceived exertion (including the concept of repetitions in reserve), with the majority devoted to periodization (including autoregulation).
Exercise principles – Individualization
Utilizing a case formulation for the person living with pain requires the clinician to make decisions based on the individuals predictive model, their preferences and to work out probable pathways that fits or expands their perceived limits. This method requires the clinician to continuously ask reflective questions such as: Why is this person presenting in this way at this time? What can be done to reduce distress and disability? How can I get the person going again? As we are dealing with human beings we need to be aware of the impact of context and that individual circumstances continuously change, hence the exercise training principle of indiviualization.
The Individualization principle refers to variability in all individuals. Katch, McArdle, & Katch, (2011) state ‘all individuals do not respond similarly to a given training stimulus’. This is essentially re-iterating the message that context matters. That appraisal of a situation will vary from person to person and so working with people living with pain means that pain management programs must meet individual needs and capacities.
Exercise Principles – Periodization
One of the original training concepts within periodization comes from Thomas Delorme’s work into progressive resistance exercise (PRE) (Delorme & Watkins, 1948). The model of PRE was based around the familiar 3 sets of 10 repetitions. It was structured so set one was to be done at 50% of the patient’s 10RM, set two at 75%, and finally set three at 100% of 10RM. Once a patient could perform greater than 10 repetitions on the final set, the weights were “progressed” accordingly (Todd, Shurley, & Todd, 2012). The format is similar to that of Fordyce’s graded activity model.
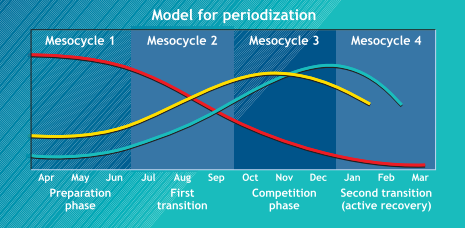
Periodization evolved to what is now understood as linear periodization (LP), a breakdown of a macrocycle (1 year), into mesocycles (separating a year into cycles based upon training and competition phases, this could be monthly), and microcycles (weekly), in which intensity gradually increases and volume gradually decreases within and between cycles (Figure. 2) (Bryan Mann, Thyfault, Ivey, & Sayers, 2010; Katch, McArdle, & Katch, 2011).

This means that load tends to increase and the number of repetitions or sets goes down the closer the individual gets to competition. An issue I have with this approach, if it were implemented within a pain management program, is that the focus is based on a hypertrophy model potentially leading to a misconception that building strength can attenuate pain. Something I have discussed in previous blogs. Now, I won’t deny that there are plenty of studies out there that have utilized an LP approach with success. For example, a systematic review (Kristensen & Franklyn-Miller, 2012)examined the effects of resistance training (RT) in various musculoskeletal conditions. In particular, the authors looked at chronic low back pain, chronic tendinopathy, knee osteoarthritis, hip replacement surgery and ACL reconstruction, concluding several major findings:
- RT is a valid therapeutic tool in the treatment of the most common musculoskeletal injuries, especially those of a chronic variety.
- RT is effective across age and gender.
- A high-intensity approach (>70% of 1RM) appears to be more effective than a low-intensity approach.
- High-intensity RT training does not increase the likelihood of injury, provided that patients are gradually introduced to heavier loads through periodised RT.
The SR identified that pain intensity did reduce in the majority of the studies and so whilst this sounds positive, it is unclear (without reading all the papers!) what clinical phenomena or features of chronic pain were part of the inclusion criteria. I’m talking things like pain related fear, pain related anxiety, avoidance behavior.
The review does mention a study ‘by Helmhout et al (2004) comparing high- and low-intensity lumbar strengthening programmes showing greater strength gains with a high-intensity approach but less reduction in kinesiophobia, prompting the authors to conclude that high-intensity RT offered no added benefits over low-intensity RT in restoring back function in CLBP. ‘ This raises some questions around the utility of using a strength focused periodization approach to pain management programs, particularly if behavioral factors are evident from clinical findings.
So as an example, can we postulate for people living with pain, if undergoing a values based pain management program, utilizing periodization will further facilitate improved outcomes in prognostic factors such as increases in self-efficacy, decreases in distress, and improvements in disability?
I work closely with Occupational Therapists (OTs) who tend to manage return to work caseloads. The utility of periodization could potentially facilitate continuity of care, transparency of communication, interdisciplinary working and developing programs. Periodization in this case may also provide a transition from a pain management program to a return to work program, thus supporting an individual to re-enter the workforce. Of course, we would expect this type of approach to be established, unfortunately there are many health professionals that still work within their individual silos.
However, the literature discussing LP has highlighted a lack of clarity regarding what type of periodization is most effective (Bryan Mann et al., 2010; Katch et al., 2011). Confounding factors include controlling for individualization, training volume and participant’s fitness capacities (Katch, McArdle, & Katch, 2011). This is primarily reflected within the exercise training literature. To my knowledge there is nothing like this in the pain management literature. However, it could be hypothesised that those same confounding factors would exist in pain management programs. In addition, there are likely confounding factors in additional variables such as fear avoidance, pain related anxiety, risk of flare up, deconditioning etc. Questions that comes from this might be, “if we are experiencing confounding variables using periodization then 1) how might we use it? and 2) what might it look like?”
Periodization – Autoregulation
One such method of periodization is autoregulation. Autoregulation differs somewhat to LP in that it adjusts to the individual’s adaptations on a day-to-day or week to week basis rather than taking a linear approach to decreasing volume and increasing intensity. This makes sense as pain management programs should not be solely focussed on a hypertrophy model and should consider the ever-changing contextual factors. Bryan Mann et al., (2010) explain, ‘this type of periodization allows the athlete to increase strength at their own pace by catering the program to the athlete’s individual strength or performance on a daily basis.’This sounds like an approach that could be adapted and potentially accommodate the variability of possible mechanisms and clinical phenomena that we acquire through case formulation. Furthermore, Ormsbee et al., (2019) acknowledges that traditional programs of periodization are designed around resistance training and do not account for physiological fluctuations such as sleep patterns and recovery. This is encouraging, as is the case in pain management programs these factors and others can contribute to flare ups.
Moreover, Ormsbee and colleagues highlight, ‘since previous data supports that recovery from exercise and the rate of adaptation to training is athlete specific, an individualized feedback-regulated model could allow for alteration of training load based upon daily readiness rather than load prescription solely based on an initial 1RM test.’ Dissecting the paragraph and examining some of the terminology used, I believe we can find comparisons similar to the pain management literature. Sentences such as ‘rate of adaptation to training is athlete specific’, ‘individualized feedback-regulated model’and ‘alteration of training load based upon daily readiness’ makes me ponder on how we may use autoregulation to complement a case formulaic approach to pain management.
To give us some idea on how we might do this I refer readers to figure 3. This is an example of a case formulation. It identifies possible selected mechanisms from a sociopsychobiological perspective and clinical phenomena in terms of how and why an individual might be presenting in the way that they do at that time. In addition, I have attempted to add a colour coding to highlight physiological aspects of physical health and behaviour and offered considerations towards their management through a periodized – autoregulated approach.

Individual feedback
If you have read my other blogs you might have noticed that I am a fan of using rate of perceivd exertion (RPE) and other feedback scales. Historically, it was Gunnar Borg that developed RPE and since it’s creation it has been associated as a subjective scale to monitor aerobic exercise intensity (Katch, McArdle, & Katch, 2011). The utility of RPE as a feedback method has been researched extensively for exercise, but others have argued it’s effectiveness for other types of training (Helms, Cronin, Storey, & Zourdos, 2016; Ormsbee et al., 2019; Zourdos et al., 2016). Interestingly, it was Borg himself who stated, “There may not be one perfect scale for all kinds of subjective intensities in all kinds of situations. Perhaps we should use different scales depending upon the purpose of the study”(Borg, 1982).
A novel approach to using RPE for resistance training is the concept of repetitions in reserve (RIR) (Figure 4) for resistance training (Helms et al., 2016; Ormsbee et al., 2019; Zourdos et al., 2016). These studies have investigated use of RIR as a scale to measure subjective feedback for resistance training when compared to percentage of 1RM. All three studies suggest that the RIR-based RPE scale is effective to gauge resistance training intensity. Furthermore, all three studies discussed the method of autoregulation in combination with RPE and proposed it’s utility in delivering improved strength gains over an LP approach.

It has also been suggested that RPE could be used to monitor fear avoidant patients (Booth et al., 2017). Whilst this is a viable option, as previously quoted from Borg it would make sense to use alternative scales based upon dominant clinical phenomena. E.g. RPE for aerobic activity, RPE-RIR for resistance training or in the case of physiological anxiety the Subjective Units of Distress Scale or SUDS. What the clinician needs to do is determine from use of case formulation what the dominant feature is at the time of meeting and subsequent meetings. Indeed, Ormsbee et al., (2019) elaborate on the use of autoregulation complemented by RIR in the following quote:
‘Perhaps, the most important usage of this RPE scale is to autoregulate training load to accommodate an athlete’s daily readiness. Specifically, if an athlete is in a volume-type training block and scheduled to perform 4 sets of 8 repetitions at 70% of 1RM, which would typically result in submaximal RPEs between 5-8; however, if fatigue is present due to previous training or non-training factors (i.e.., sleep, anxiety, etc) the pre-determined sets and repetitions may not be feasible at the pre-determined training load. In this case the lifter may simply adjust training load to fall between a 5-8 RPE for 4 sets of 8 repetitions.’
Therefore, it would seem entirely possible to consider non-training factors (as mentioned above) that are extensively recognised within the context of a pain management program as part of an autoregulation periodized program.
Putting it all together
I appreciate that I have drawn information from the exercise training literature and that it is associated with athletes whom are working towards competition. However, if we think a bit more broadly and consider the clinical phenomena determined in an individual living with pain, I feel there should not be any reason why we cannot utilise the same approach. Rather than looking at specific principles of training to prepare for competition perhaps we should consider principles of distress and disability and how this is limiting people from fulfilling their values, all complemented by an autoregulation approach. In addition, a structured case formulaic approach that is values based and utilises an auto-regulated approach (to potentially mitigate the risk of flare up) may provide the additional motivation for readiness required for people living with pain. Of course, appreciating the broader context of working in pain management this approach would work best if complemented by other approaches such as motivation interviewing and cognitive behavioural therapy or acceptance and commitment therapy.
Thanks for having a read.
TNP
References:
Booth, J., Moseley, G. L., Schiltenwolf, M., Cashin, A., Davies, M., & Hübscher, M. (2017). Exercise for chronic musculoskeletal pain: A biopsychosocial approach. Musculoskeletal Care, (April). https://doi.org/10.1002/msc.1191
Borg, G. A. (1982). Psychophysical bases of perceived exertion. Medicine and Science in Sports and Exercise, 14(5), 377–381. https://doi.org/10.1249/00005768-198205000-00012
Bryan Mann, J., Thyfault, J. P., Ivey, P. A., & Sayers, S. P. (2010). THE EFFECT OF AUTOREGULATORY PROGRESSIVE RESISTANCE EXERCISE VS. LINEAR PERIODIZATION ON STRENGTH IMPROVEMENT IN COLLEGE ATHLETES. The Journal of Strength and Conditioning Research, 24(7), 1718–1723.
Delorme, T. L., & Watkins, A. L. (1948). Technics of progressive resistance exercise. Archives of Physical Medicine and Rehabilitation, 29(5), 263–273.
Fordyce, W. E. (2015). Fordyce’s Behavioural Methods for Chronic Pain and Illness. (C. J. Main, F. J. Keefe, M. P. Jensen, J. W. S. Vlaeyen, & K. E. Vowles, Eds.). Seattle: IASP Press.
Helms, E. R., Cronin, J., Storey, A., & Zourdos, M. C. (2016). Application of the Repetitions in Reserve-Based Rating of Perceived Exertion Scale for Resistance Training. Strength and Conditioning Journal, 38(4), 1. https://doi.org/10.1519/SSC.0000000000000218
Hodges, P. W. (2019). Hybrid approach to treatment tailoring for low back pain: A proposed model of care. Journal of Orthopaedic & Sports Physical Therapy, 0(0), 1–37. Retrieved from http://www.jospt.org
Katch, V. L., McArdle, W. D., & Katch, F. I. (2011). Training the Anaerobic and Aerobic Energy Systems. In Essentials of Exercise Physiology(4th Editio, pp. 409–442). Lippincott Williams & Wilkins.
Kristensen, J., & Franklyn-Miller, A. (2012). Resistance training in musculoskeletal reahbilitation: a systematic review. British Journal of Sports Medicine,46, 719–726. https://doi.org/10.1136/bjsports79376
Ormsbee, M. J., Carzoli, J. P., Klemp, A., Allman, B. R., Zourdos, M. C., Kim, J. S., & Panton, L. B. (2019). Efficacy of the Repetitions in Reserve-Based Rating of Perceived Exertion for the Bench Press in Experienced and Novice Benchers. Journal of Strength and Conditioning Research, 33(2), 337–345. https://doi.org/10.1519/JSC.0000000000001901
Todd, J. S., Shurley, J. P., & Todd, T. C. (2012). THOMAS L. DELORME AND THE SCIENCE OF PROGRESSIVE RESISTANCE EXERCISE. Journal of Strength and Conditioning Research, 26(11), 2913–2923.
Zourdos, M. C., Klemp, A., Dolan, C., Quiles, J. M., Schau, K. A., Jo, E., … Blanco, R. (2016). Novel Resistance Training-Specific Rating of Perceived Exertion Scale Measuring Repetitions in Reserve. Journal of Strength and Conditioning Research(Vol. 30). https://doi.org/10.1519/JSC.0000000000001049

Leave a reply to the naked physio Cancel reply